Introduction
Over 12,000 people are treated for new psychotic disorders across the United Kingdom and Ireland each year (Jacinto, Ding, Stafford, et al., Reference Jacinto, Ding and Stafford2023; McDonald, Ding, Ker, et al., Reference McDonald, Ding and Ker2021; Tsiachristas, Thomas, Leal, et al., Reference Tsiachristas, Thomas and Leal2016). It is common for affected individuals to be admitted to a hospital, but as of yet, the exact proportions of hospitalization at initial presentation are not known. This is important to determine because, although there are positive aspects to hospital admission in that it can offer a protective environment, foster medication compliance, and provide relief from external stressors, it can also be costly, restrictive, traumatic, and obstructive to vocational activities (Kennedy, Altar, Taylor, et al., Reference Kennedy, Altar and Taylor2014; Rodrigues & Anderson, Reference Rodrigues and Anderson2017; Zubi & Connolly, Reference Zubi and Connolly2013). Across psychiatric services, there has been a general move away from hospitalization in favor of community-based care. For first-episode psychosis (FEP) specifically, there is a growing emphasis on the utilization of early intervention services (EISs), which offer timely support to affected individuals through biological, psychological, and social treatments delivered in clinics and via assertive outreach programs (Correll, Galling, Pawar, et al., Reference Correll, Galling and Pawar2018). These services aim to reduce the duration of untreated psychosis (DUP), reduce admissions where possible, and improve functional outcomes. Despite this, studies show that admission is still common throughout the course of a psychotic illness (Ajnakina, Stubbs, Francis, et al., Reference Ajnakina, Stubbs and Francis2020; Robinson, Schooler, Rosenheck, et al., Reference Robinson, Schooler and Rosenheck2019). What is not yet known is the international proportion of people with FEP who are admitted when they first present to services. As efforts to reduce institutionalization and enhance outpatient treatment continue, a broader understanding of admissions at first presentation is required, including whether various demographic, clinical, and service-level factors have an impact.
This systematic review aimed to determine (i) the proportion of people with FEP who are admitted overall at the time of first presentation; (ii) the proportion of people with FEP who are admitted involuntarily at the time of first presentation; and (iii) the difference in the proportion admitted, if any, according to individual factors (sex), clinical factors (diagnosis and DUP), and service-level factors (EIS access).
Methods
Registration and research question framework
This review was conducted in accordance with the relevant sections of the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement (Page, McKenzie, Bossuyt, et al., Reference Page, McKenzie and Bossuyt2021) and was prospectively registered with PROSPERO International Prospective Register of Systematic Reviews (CRD42023441984) with details available at: http://www.crd.york.ac.uk/prospero. The research question was established using the Population, Exposure, and Outcome framework – the population being individuals of any age, the exposure being FEP, and the outcome being hospital admission.
Eligibility criteria
Inclusion criteria
This review included studies that had participants with a clinical, research, or registry diagnosis of FEP. Types of studies included observational studies (cohort, case–control, and cross-sectional) and interventional studies (randomized controlled trials and nonrandomized controlled trials), but only preintervention data were considered. This review included all studies evaluating the proportion of people admitted at the time of first presentation in FEP, specifically referring to admissions within 30 days of presenting to services. The 30-day timeframe was chosen to allow for the fact that there can be delays to admission for several reasons, including staggered initial assessments, diagnostic uncertainty, the need for acceptance by the appropriate hospital, and the orchestration of involuntary admissions. The inclusion criteria were as follows: (i) studies that had participants of any age with any psychotic illness (affective and nonaffective); (ii) studies that had participants with comorbid alcohol/substance use or intellectual disability, and (iii) studies that had been peer-reviewed and published in the English language.
Exclusion criteria
This review did not include case reports, case series, or systematic reviews/meta-analyses.
Search strategy
The search strategy was developed by two reviewers (L.G. and B.O’D.) in consultation with a college librarian. The following databases were searched from inception until June 1, 2023: PubMed, Embase, PsycINFO, and CINAHL. The keywords used were (“first episode” OR “first-episode” OR “acute”) AND (“psychosis” OR “psychoses” OR “psychotic” OR “schiz*”) AND (“admission*” OR “admitted” OR “hospitalisation” OR “hospitalization” OR “hospital*” OR “detention*” OR “detained” OR “committed” OR “ward*” OR “unit*” OR “inpatient”). The reference lists of the included articles were manually searched. See Supplementary Figure 1 for the complete search strategy.
Titles and abstracts of potentially eligible articles were screened independently by two reviewers (L.G. and V.T.). Inclusion criteria were applied, and any disagreements that arose were resolved through consensus with a third reviewer (B.O’D.). Full texts of selected articles were then screened independently by two reviewers (L.G. and V.T.), and any disagreements were again resolved through consensus with a third reviewer (B.O’D.). The authors were contacted if further clarity or data relating to the articles was required. Covidence software was used.
Data extraction
Data extraction commenced on September 22, 2023, and was completed independently by two reviewers (L.G. and V.T.). Consensus was achieved with a third reviewer (B.O’D.). Relevant general data extracted for each study included first author, year, country, sample size, aim, design, duration, eligibility criteria, data sources, diagnostic tools used, and the presence or absence of an EIS. An EIS was deemed to be present if stated in the study. Regarding the primary outcomes of the systematic review, relevant data included the proportion of participants admitted to the hospital overall at first presentation and the proportion admitted involuntarily. Regarding these outcomes, the number of overall admissions and involuntary admissions was extracted as a proportion of the entire study cohort. Demographic population characteristics included age, sex, marital status, employment/education status, and ethnicity/migrant status. Clinical population characteristics included diagnosis, DUP, risk of self-harm or violence, severity of psychopathology, and alcohol/substance use.
For three studies, data regarding the primary outcome of the proportion admitted were obtained through contact with authors (Baumann, Crespi, Marion-Veyron, et al., Reference Baumann, Crespi and Marion-Veyron2013; Belvederi Murri, Bertelli, Carozza, et al., Reference Belvederi Murri, Bertelli and Carozza2021; Oduola, Craig, & Morgan, Reference Oduola, Craig and Morgan2021). For one of these, the data that was provided pertained to the defined study duration (Oduola et al., Reference Oduola, Craig and Morgan2021). For the other two, authors provided recent data enabling a more up-to-date analysis, encompassing data from 2012 until 2024 (Belvederi Murri et al., Reference Belvederi Murri, Bertelli and Carozza2021), and from 2004 until 2023 (Baumann et al., Reference Baumann, Crespi and Marion-Veyron2013). For studies in which participants started out as either inpatients or outpatients, this was interpreted as the inpatient cohort having been admitted at the time of presentation. See Supplementary Figure 2 for further details on the data extraction process.
Study risk of bias assessment
The National Institutes of Health (NIH) Quality Assessment Tool was used to assess the quality and risk of bias for all studies (Jiu, Hartog, Wang, et al., Reference Jiu, Hartog and Wang2024). This tool was chosen because it is designed for the assessment of observational studies. It assesses studies across 13 domains, including research question, population, participation, group comparability, sample size, point of exposure measurement (i.e. before outcome), timeframe, exposure levels, outcome measurement, blinding, follow-up, adjustment for confounding, and statistical analysis. Each domain is scored as yes, no, unclear, or not applicable to provide an overall quality rating for each study as good, fair, or poor. For the purpose of this review, certain domains were deemed not applicable. These included group comparability (as the research question only applied to one group, i.e. people with FEP), follow-up (as the research question related only to first contact), and blinding and adjustment for confounding (as these would not be relevant to the research question).
Data analysis
The meta-analysis was conducted with Stata/BE 18 statistical software (StataCorp, n.d.). The pooled proportion of people admitted at the time of presentation was calculated using a random-effects model (Dettori, Norvell, & Chapman, Reference Dettori, Norvell and Chapman2022). This was first done for (i) all admissions and subsequently for (ii) involuntary admissions, in each case as a proportion of the entire study cohort. To examine the potential impact of having access to an EIS on these primary outcomes, the analyses were further stratified according to the presence or absence of an EIS. Where data were available, subgroup analyses according to demographic and clinical characteristics were also conducted. This was done for (i) sex, (ii) diagnosis, and (iii) DUP. One of the study’s aims was to conduct a subgroup analysis according to migrant status; however, the data were not available across studies to make this possible. A p-value of <0.05 was set as statistically significant. The I 2 statistic was used to represent heterogeneity, with a value above 75% indicating high heterogeneity (Higgins, Thompson, Deeks, et al., Reference Higgins, Thompson and Deeks2003). The summary statistics were illustrated with forest plots (Dettori, Norvell, & Chapman, Reference Dettori, Norvell and Chapman2021). A funnel plot was considered to assess for publication bias; however, this is not recommended for use in meta-analyses of proportions (Cheema, Shahid, Ehsan, et al., Reference Cheema, Shahid and Ehsan2022).
Results
Search results
The initial search yielded 8,203 articles. After the removal of duplicates, 7,455 articles remained. Following title and abstract screening, 168 articles were deemed eligible for full text review. At this stage, 50 authors were contacted for further information, and 21 responses were received (see the Acknowledgments section). A total of 25 articles met eligibility criteria (Ayesa-Arriola, Rodríguez-Sánchez, Morelli, et al., Reference Ayesa-Arriola, Rodríguez-Sánchez and Morelli2011; Baumann et al., Reference Baumann, Crespi and Marion-Veyron2013; Belvederi Murri et al., Reference Belvederi Murri, Bertelli and Carozza2021; Chang, Lau, Chiu, et al., Reference Chang, Lau and Chiu2016; Chang, Tang, Hui, et al., Reference Chang, Tang and Hui2012; Chen, Tang, Hui, et al., Reference Chen, Tang and Hui2011; Doré-Gauthier, Miron, Jutras-Aswad, et al., Reference Doré-Gauthier, Miron and Jutras-Aswad2020; Drake, Caton, Xie, et al., Reference Drake, Caton and Xie2011; Greenfield, Joshi, Christian, et al., Reference Greenfield, Joshi and Christian2018; Guitter, Laprevote, Lala, et al., Reference Guitter, Laprevote and Lala2021; Hui, Chiu, Li, et al., Reference Hui, Chiu and Li2015; Hui, Lau, Leung, et al., Reference Hui, Lau and Leung2015; Hui, Poon, Kwok, et al., Reference Hui, Poon and Kwok2015; Keane, Szigeti, Fanning, et al., Reference Keane, Szigeti and Fanning2019; Kurdyak, Mallia, de Oliveira, et al., Reference Kurdyak, Mallia and de Oliveira2021; Larsen, Friis, Haahr, et al., Reference Larsen, Friis and Haahr2004; O’Callaghan, Turner, Renwick, et al., Reference O’Callaghan, Turner and Renwick2010; O’Donoghue, Collett, Boyd, et al., Reference O’Donoghue, Collett and Boyd2022; O’Donoghue, Roche, Lyne, et al., Reference O’Donoghue, Roche and Lyne2023; Oduola et al., Reference Oduola, Craig and Morgan2021; Qin, Zhang, Wang, et al., Reference Qin, Zhang and Wang2014; Roche, Lyne, O’Donoghue, et al., Reference Roche, Lyne and O’Donoghue2015; Roche, Lyne, O’Donoghue, et al., Reference Roche, Lyne and O’Donoghue2016; Vazquez-Barquero, Cuesta Nunez, De la Varga, et al., Reference Vazquez-Barquero, Cuesta Nunez and De la Varga1995; Waxmann, Thompson, McGorry, et al., Reference Waxmann, Thompson and McGorry2022) and screening of these reference lists did not identify any further relevant studies. Seven articles were further excluded due to overlap of study populations (Chang et al., Reference Chang, Lau and Chiu2016), in which cases the studies with larger sample sizes were kept for inclusion. Those excluded due to the overlap were used for secondary analysis where needed. This resulted in a final total of 18 articles. One of these was a study by Waxmann et al. (Reference Waxmann, Thompson and McGorry2022), but a more recent study by Gannon, Mullen, McGorry, et al. (Reference Gannon, Mullen and McGorry2023) examined the same patient cohort and was, therefore, included instead to reflect more up-to-date findings. A summary of the search is displayed in the PRISMA flow chart (Figure 1). Characteristics of the 18 included studies (Ayesa-Arriola et al., Reference Ayesa-Arriola, Rodríguez-Sánchez and Morelli2011; Baumann et al., Reference Baumann, Crespi and Marion-Veyron2013; Belvederi Murri et al., Reference Belvederi Murri, Bertelli and Carozza2021; Chen et al., Reference Chen, Tang and Hui2011; Doré-Gauthier et al., Reference Doré-Gauthier, Miron and Jutras-Aswad2020; Drake et al., Reference Drake, Caton and Xie2011; Gannon et al., Reference Gannon, Mullen and McGorry2023; Greenfield et al., Reference Greenfield, Joshi and Christian2018; Guitter et al., Reference Guitter, Laprevote and Lala2021; Hui, Lau, et al., Reference Hui, Lau and Leung2015; Keane et al., Reference Keane, Szigeti and Fanning2019; Kurdyak et al., Reference Kurdyak, Mallia and de Oliveira2021; Larsen et al., Reference Larsen, Friis and Haahr2004; O’Donoghue et al., Reference O’Donoghue, Collett and Boyd2022; Oduola et al., Reference Oduola, Craig and Morgan2021; Qin et al., Reference Qin, Zhang and Wang2014; Roche et al., Reference Roche, Lyne and O’Donoghue2015; Vazquez-Barquero et al., Reference Vazquez-Barquero, Cuesta Nunez and De la Varga1995) are displayed in Table 1.
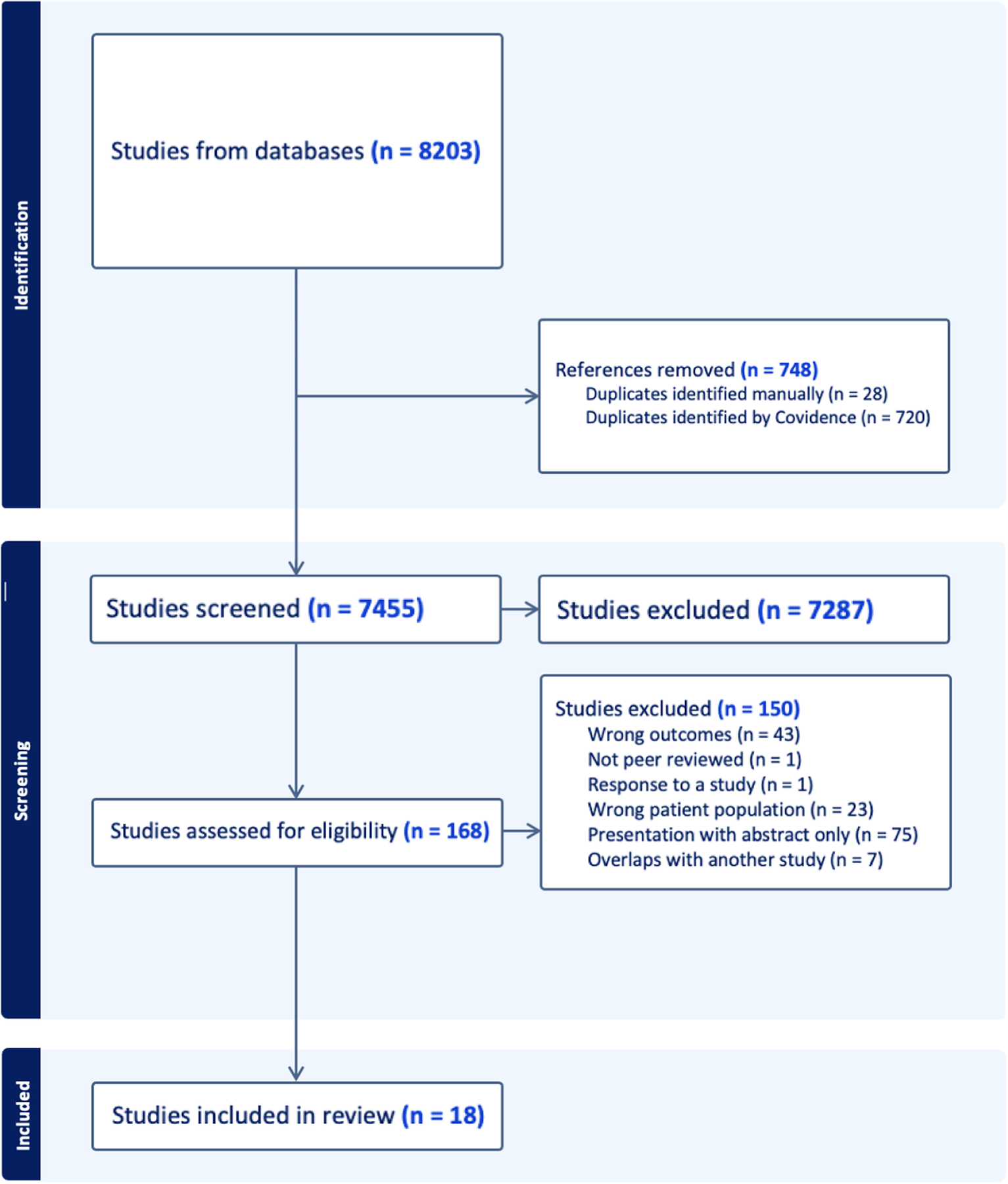
Figure 1. PRISMA flow chart.
Table 1. Characteristics of included studies

* CAARMS, Comprehensive Assessment of At Risk Mental States; *ICD 9, International Classification of Diseases, ninth edition; *ICD 10, International Classification of Diseases, 10th edition; *DSM IV, Diagnostic and Statistical Manual of Mental Disorders, fourth edition, *SCID IV, Structured Clinical Interview for DSM IV; *CCMD 3, Chinese Classification of Mental Disorders, third edition; *PRISM IV, Psychiatric Research Interview for Substance and Mental Disorders for DSM IV; *DSM-IIIR, Diagnostic and Statistical Manual of Mental Disorders, third edition, revised; *Scale for the Assessment of Positive Symptoms, *Health of the Nation Outcome Scales, *Social and Occupational Functioning Assessment Scale, *Global Assessment of Functioning, *Clinical Global Impression Severity Scale, *Scale for the Assessment of Negative Symptoms, *Positive and Negative Syndrome Scale, *Brief Psychiatric Rating Scale.
Characteristics of included studies
Sample size: Across the 18 included studies, the total sample size was 19,854 participants.
Year: Years of publication ranged from 1995 to 2023.
Design: Regarding study design, 14 were cohort studies (Ayesa-Arriola et al., Reference Ayesa-Arriola, Rodríguez-Sánchez and Morelli2011; Baumann et al., Reference Baumann, Crespi and Marion-Veyron2013; Belvederi Murri et al., Reference Belvederi Murri, Bertelli and Carozza2021; Doré-Gauthier et al., Reference Doré-Gauthier, Miron and Jutras-Aswad2020; Drake et al., Reference Drake, Caton and Xie2011; Gannon et al., Reference Gannon, Mullen and McGorry2023; Greenfield et al., Reference Greenfield, Joshi and Christian2018; Guitter et al., Reference Guitter, Laprevote and Lala2021; Hui, Lau, et al., Reference Hui, Lau and Leung2015; Kurdyak et al., Reference Kurdyak, Mallia and de Oliveira2021; Larsen et al., Reference Larsen, Friis and Haahr2004; O’Donoghue et al., Reference O’Donoghue, Collett and Boyd2022; Oduola et al., Reference Oduola, Craig and Morgan2021; Qin et al., Reference Qin, Zhang and Wang2014), 2 were cross-sectional studies (Keane et al., Reference Keane, Szigeti and Fanning2019; Vazquez-Barquero et al., Reference Vazquez-Barquero, Cuesta Nunez and De la Varga1995), 1 was a cross-validation study (Roche et al., Reference Roche, Lyne and O’Donoghue2015), and 1 was a case–control study (Chen et al., Reference Chen, Tang and Hui2011).
Country: Three studies were conducted in China (Chen et al., Reference Chen, Tang and Hui2011; Hui, Lau, et al., Reference Hui, Lau and Leung2015; Qin et al., Reference Qin, Zhang and Wang2014), two in Canada (Doré-Gauthier et al., Reference Doré-Gauthier, Miron and Jutras-Aswad2020; Kurdyak et al., Reference Kurdyak, Mallia and de Oliveira2021), two in Australia (Gannon et al., Reference Gannon, Mullen and McGorry2023; O’Donoghue et al., Reference O’Donoghue, Collett and Boyd2022), two in Spain (Ayesa-Arriola et al., Reference Ayesa-Arriola, Rodríguez-Sánchez and Morelli2011; Vazquez-Barquero et al., Reference Vazquez-Barquero, Cuesta Nunez and De la Varga1995), two in the United Kingdom (Greenfield et al., Reference Greenfield, Joshi and Christian2018; Oduola et al., Reference Oduola, Craig and Morgan2021), two in Ireland (Keane et al., Reference Keane, Szigeti and Fanning2019; Roche et al., Reference Roche, Lyne and O’Donoghue2015), and the remainder were conducted in Switzerland (Baumann et al., Reference Baumann, Crespi and Marion-Veyron2013), Italy (Belvederi Murri et al., Reference Belvederi Murri, Bertelli and Carozza2021), France (Guitter et al., Reference Guitter, Laprevote and Lala2021), Norway (Larsen et al., Reference Larsen, Friis and Haahr2004), and the United States (Drake et al., Reference Drake, Caton and Xie2011).
Diagnostic tools: Diagnostic tools used included the Structured Clinical Interview for the Diagnostic and Statistical Manual of Mental Disorders, fourth edition (DSM IV) (Ayesa-Arriola et al., Reference Ayesa-Arriola, Rodríguez-Sánchez and Morelli2011; Hui, Lau, et al., Reference Hui, Lau and Leung2015; Keane et al., Reference Keane, Szigeti and Fanning2019; Larsen et al., Reference Larsen, Friis and Haahr2004; Roche et al., Reference Roche, Lyne and O’Donoghue2015), DSM IV (Doré-Gauthier et al., Reference Doré-Gauthier, Miron and Jutras-Aswad2020; Kurdyak et al., Reference Kurdyak, Mallia and de Oliveira2021), DSM, third edition, revised (DSM IIIR) (Vazquez-Barquero et al., Reference Vazquez-Barquero, Cuesta Nunez and De la Varga1995), the International Classification of Diseases (ICD) (Oduola et al., Reference Oduola, Craig and Morgan2021), ICD, 10th edition (ICD-10) (Chen et al., Reference Chen, Tang and Hui2011; Greenfield et al., Reference Greenfield, Joshi and Christian2018; Guitter et al., Reference Guitter, Laprevote and Lala2021), ICD, ninth edition (ICD-9) (Belvederi Murri et al., Reference Belvederi Murri, Bertelli and Carozza2021; Kurdyak et al., Reference Kurdyak, Mallia and de Oliveira2021; Vazquez-Barquero et al., Reference Vazquez-Barquero, Cuesta Nunez and De la Varga1995), the Comprehensive Assessment of At-Risk Mental States (Baumann et al., Reference Baumann, Crespi and Marion-Veyron2013; Gannon et al., Reference Gannon, Mullen and McGorry2023; O’Donoghue et al., Reference O’Donoghue, Collett and Boyd2022), the Psychiatric Research Interview for Substance and Mental Disorders for DSM IV (Drake et al., Reference Drake, Caton and Xie2011), and the Chinese Classification of Mental Disorders, third edition (Qin et al., Reference Qin, Zhang and Wang2014).
Quality assessment: A total of 13 studies met the criteria for good overall quality, and five met the criteria for fair overall quality, as per the NIH Quality Assessment Tool. See Supplementary Figure 3 for the complete quality assessment.
Studies with data regarding different subgroups
Legal status of admission: Six studies reported data on the proportion of people who were involuntarily admitted, comprising a total sample size of 2,999 participants (Gannon et al., Reference Gannon, Mullen and McGorry2023; Guitter et al., Reference Guitter, Laprevote and Lala2021; Keane et al., Reference Keane, Szigeti and Fanning2019; O’Donoghue et al., Reference O’Donoghue, Collett and Boyd2022; Oduola et al., Reference Oduola, Craig and Morgan2021; Roche et al., Reference Roche, Lyne and O’Donoghue2015).
Service level factors: A total of 10 studies had EIS access (Ayesa-Arriola et al., Reference Ayesa-Arriola, Rodríguez-Sánchez and Morelli2011; Baumann et al., Reference Baumann, Crespi and Marion-Veyron2013; Belvederi Murri et al., Reference Belvederi Murri, Bertelli and Carozza2021; Doré-Gauthier et al., Reference Doré-Gauthier, Miron and Jutras-Aswad2020; Gannon et al., Reference Gannon, Mullen and McGorry2023; Greenfield et al., Reference Greenfield, Joshi and Christian2018; Hui, Lau, et al., Reference Hui, Lau and Leung2015; Keane et al., Reference Keane, Szigeti and Fanning2019; O’Donoghue et al., Reference O’Donoghue, Collett and Boyd2022; Roche et al., Reference Roche, Lyne and O’Donoghue2015), while five studies did not. (Drake et al., Reference Drake, Caton and Xie2011; Guitter et al., Reference Guitter, Laprevote and Lala2021; Kurdyak et al., Reference Kurdyak, Mallia and de Oliveira2021; Qin et al., Reference Qin, Zhang and Wang2014; Vazquez-Barquero et al., Reference Vazquez-Barquero, Cuesta Nunez and De la Varga1995) Two studies contained mixed population samples – some with EIS access and some without (Larsen et al., Reference Larsen, Friis and Haahr2004; Oduola et al., Reference Oduola, Craig and Morgan2021), and one study compared two groups pre- and post-implementation of an EIS (Chen et al., Reference Chen, Tang and Hui2011). For this subgroup analysis, the study comparing two groups pre- and post-EIS was analyzed as two separate cohorts (Chen et al., Reference Chen, Tang and Hui2011). Theoretically, one of the EIS studies also compared two groups pre- and post-EIS, but due to study overlap regarding the historical pre-EIS cohort, this was treated as an EIS cohort only throughout the systematic review (Keane et al., Reference Keane, Szigeti and Fanning2019). The two studies that comprised mixed populations (Larsen et al., Reference Larsen, Friis and Haahr2004; Oduola et al., Reference Oduola, Craig and Morgan2021) were not included in the EIS subgroup analysis.
Demographic factors: Three studies reported data on sex in relation to admission (Gannon et al., Reference Gannon, Mullen and McGorry2023; Kurdyak et al., Reference Kurdyak, Mallia and de Oliveira2021; Vazquez-Barquero et al., Reference Vazquez-Barquero, Cuesta Nunez and De la Varga1995). This data applies to overall admissions only, and not to involuntary admissions. Migrant status, ethnicity, and age were reported in some studies, but could not be included in the meta-analysis due to inconsistencies in how data were measured and presented across studies.
Clinical factors: Two studies reported data on diagnosis in relation to admission (Chang et al., Reference Chang, Lau and Chiu2016; Gannon et al., Reference Gannon, Mullen and McGorry2023), and two studies reported data on DUP in relation to admission (Chang et al., Reference Chang, Tang and Hui2012; Gannon et al., Reference Gannon, Mullen and McGorry2023). In both cases, one of the two studies used in this secondary analysis was initially excluded from the primary analysis due to study overlap (Chang et al., Reference Chang, Tang and Hui2012; Chang et al., Reference Chang, Lau and Chiu2016). Both studies relate to the study by Chen et al., which was used in the primary analysis (Chen et al., Reference Chen, Tang and Hui2011). This data applies to overall admissions only and not to involuntary admissions.
Proportion of people admitted at the time of presentation
Overall and involuntary admissions
Across the 18 included studies, the pooled proportion of people admitted overall at the time of first presentation was just over half, at 51% (95% CI = 37–65%; I 2 = 99.56%). These results are presented in Figure 2. Across the studies that reported data on legal status (k = 6), the pooled proportion of people admitted involuntarily at the time of first presentation was just under one-third, at 31% (95% CI = 23–40%; I 2 = 95.26%). Within these six studies, 54.0% (1,621/2,999) of people were admitted overall, and of these admissions, 55.2% (895/1,621) were involuntary. These results are presented in Figure 3.
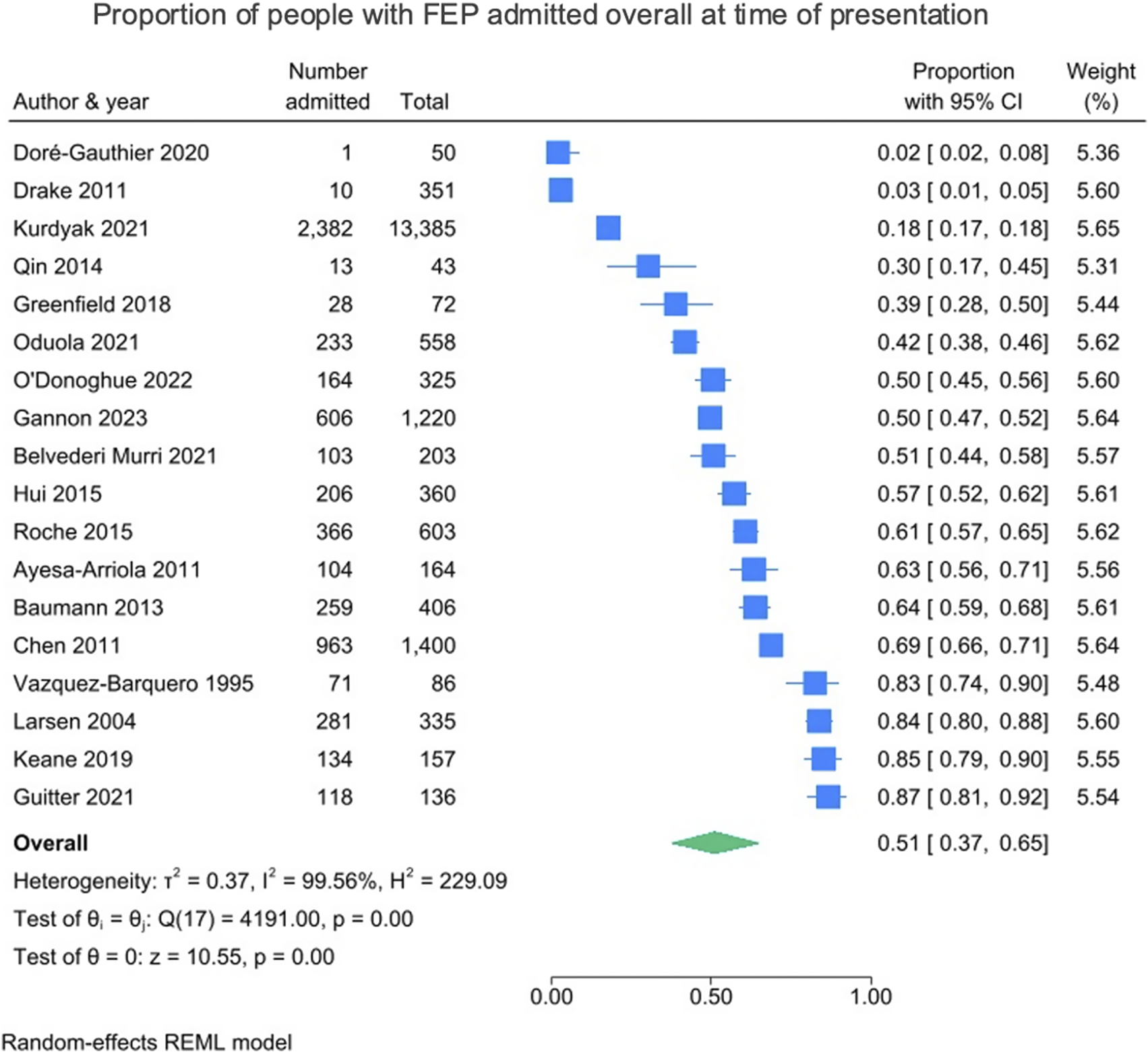
Figure 2. Proportion of people with FEP admitted overall at time of presentation.
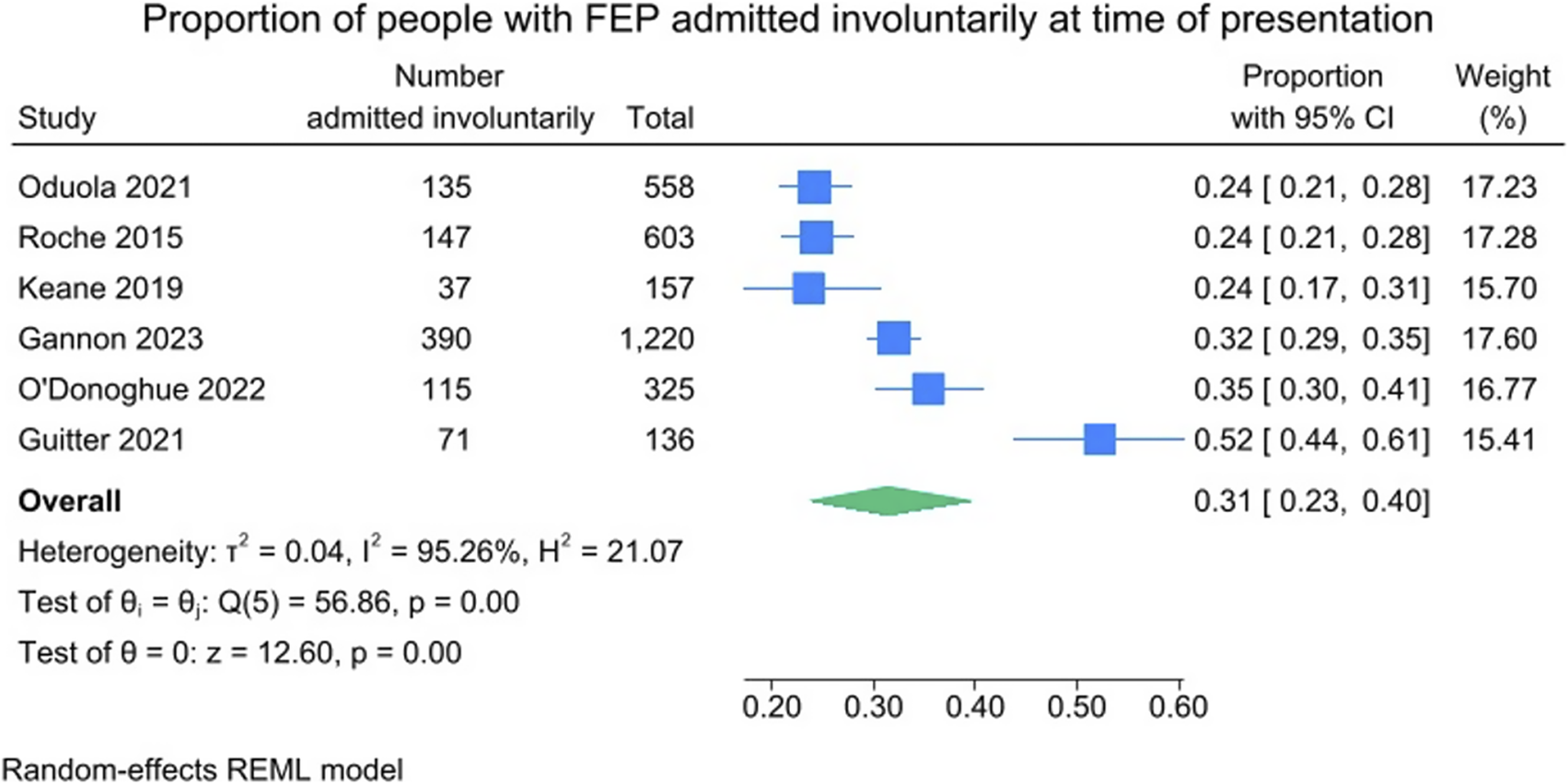
Figure 3. Proportion of people with FEP admitted involuntarily at time of presentation.
Early intervention services
Regarding the studies in which participants had access to an EIS (k = 10), the pooled proportion of people admitted overall at the time of first presentation was 48% (95% CI = 35–60%), and without EIS access (k = 7), the proportion admitted was 57% (CI = 25–86%), with no statistically significant difference found between the two groups (p = 0.62). These results are presented in Figure 4. Where participants had access to an EIS, the pooled proportion of people admitted involuntarily at the time of first presentation was 30% (95% CI = 24–37%), and without EIS access, the proportion admitted involuntarily was 37% (95% CI = 12–66%), with no statistically significant difference found between the two groups (p = 0.63). These results are presented in Supplementary Figure 4.

Figure 4. Proportion of people with FEP admitted overall at time of presentation, according to EIS access.
Admissions according to sex, diagnosis, and DUP
Across the studies which reported on sex in relation to admission (k = 3), the proportion of people admitted overall at the time of first presentation was 53% in males (95% CI = 15–89%) and 45% in females (95% CI = 12–81%), with no statistically significant difference found between the two groups (p = 0.80) (see Supplementary Figure 5). Regarding diagnosis (k = 2), the proportion of people with nonaffective psychosis admitted overall at the time of first presentation was 48% (95% CI = 45–51%), and the proportion of people with affective psychosis admitted was 74% (95% CI = 39–97%), with no statistically significant difference found between the two groups (p = 0.14) (see Supplementary Figure 6). For DUP (k = 2), the proportion of people with a short DUP (<3 months) admitted overall at the time of first presentation was 59% (95% CI = 56–63%), and the proportion of people with a long DUP (>3 months) admitted was 37% (95% CI = 33–41%), with a statistically significant difference noted between the two groups (p < 0.001) (see Supplementary Figure 7).
Discussion
Main findings
In FEP, the proportion of people admitted to hospital overall at the time of first presentation is just over half, at 51%, and 31% of individuals who present are admitted involuntarily. Subgroup analyses found that a higher proportion of individuals with a short DUP are admitted (defined as <3 months), compared to those with a longer DUP (59% vs. 37%). There were no significant differences found according to sex, diagnosis, or access to early intervention for psychosis services.
Strengths and limitations
To our knowledge, this is the first meta-analysis on the proportion of people with FEP admitted at the time of first presentation. The initial search yielded a substantial number of articles, representing a thorough search of the literature. A large number of studies were included with a comprehensive total sample size, comprising several different countries, and all studies met criteria for good overall quality. However, the results must be interpreted in the context of some limitations. Regarding the main outcome, it is possible that studies not included in this meta-analysis could have reported on early admissions in FEP as descriptive data, but if not stated in the abstract, such studies would not have been identified. Regarding included studies, there was high heterogeneity between them, and low- and middle-income countries were underrepresented, which may mean results are not generalizable on a global level. Regarding the variables examined, only six studies reported on the legal status of admission; numbers in the subgroup analyses for sex, diagnosis, and DUP were low; and there were insufficient data to conduct a subgroup analysis for ethnicity/migrant status or age, both often linked to psychiatric admission risk (in general and in FEP).
Heterogeneity
As mentioned above, a high degree of heterogeneity was observed among included studies, which could be due to several factors. First, there were demographic differences between some of the cohorts studied. For example, Doré-Gauthier et al. looked exclusively at homeless youth (Doré-Gauthier et al., Reference Doré-Gauthier, Miron and Jutras-Aswad2020) and Greenfield et al. looked exclusively at the over-35 years age category (Greenfield et al., Reference Greenfield, Joshi and Christian2018), both representing important social factors differentiating these cohorts from a more generalizable group. Second, clinical differences among participants could have had an impact on admission requirements, that is, differing levels of symptom severity and indeed differing diagnostic subcategories. Third, attitudes toward hospitalization in psychiatry are ever-changing, and some studies were conducted several years ago, including cohorts from 1989 to 1991 (Vazquez-Barquero et al., Reference Vazquez-Barquero, Cuesta Nunez and De la Varga1995), 1993 to 1994 (Larsen et al., Reference Larsen, Friis and Haahr2004), and 1995 to 1998 (Keane et al., Reference Keane, Szigeti and Fanning2019). Fourth, in certain studies, individuals within the cohort were separated into inpatients and outpatients from the outset, that is, they were already admitted for FEP when the study started (Keane et al., Reference Keane, Szigeti and Fanning2019; Kurdyak et al., Reference Kurdyak, Mallia and de Oliveira2021; Roche et al., Reference Roche, Lyne and O’Donoghue2015; Vazquez-Barquero et al., Reference Vazquez-Barquero, Cuesta Nunez and De la Varga1995). We interpreted this as admission at initial presentation, but it should be noted as a variation in methodology. Finally, cultural differences must be taken into account. Studies were conducted across a variety of countries, all of which have different processes, standards, and availability of resources. There are several practical considerations when making decisions regarding hospital admission, and these factors inevitably vary from country to country, and indeed from service to service. Guitter et al. noted that France has a significant delay in the development of early intervention centers (Guitter et al., Reference Guitter, Laprevote and Lala2021). In areas that have EIS access, these services also exhibit variations in how they operate, discussed in further detail below.
Implications
Early intervention services
In this study, access to an EIS did not have a significant impact on the proportion of admissions at presentation, overall or involuntary. This could be considered surprising, as it may be expected that the intensive community care offered in EISs would drive admissions down. Indeed, a 2015 meta-analysis on the effect of early interventions for psychosis on the usage of inpatient services found that early intervention programs significantly reduced admissions during follow-up (Randall, Vokey, Loewen, et al., Reference Randall, Vokey and Loewen2015). However, the distinction between admissions during follow-up and admissions at first presentation is important, and for this systematic review, results must be interpreted with an allowance for the heterogeneity between various EIS systems. For example, the Dublin and East Treatment and Early Care Team (DETECT) EIS in Ireland initially provides a consultation service while the patient remains under the official care of their community mental health team. In fact, patients are only referred to DETECT by community mental health teams after the first presentation, at which point the decision regarding treatment setting (inpatient vs outpatient) has usually already been made. This differs from the Early Psychosis Prevention and Intervention Centre EIS in Australia, where patients may be referred via a multitude of pathways, including primary care, family members, or self, in which cases an influence on early admission figures may be observed. EISs work according to different models; some are hub and spoke, others standalone, and additionally, differences are likely to exist between the wider community services in which they are situated.
Duration of untreated psychosis
Worth noting in this review is the difference in the proportion of people admitted depending on DUP. Those with a short DUP (<3 months) were significantly more likely to be hospitalized when they first presented. This is possibly due to the more acute and sometimes alarming presentations that can occur in the context of a short DUP, in contrast to individuals with a long DUP, who tend to present in a more insidious manner. When the decision is being made regarding inpatient versus outpatient care, it is important that both of these groups are catered for, and that each person’s specific treatment targets are considered, whether or not the presentation is extreme in nature. We know that a longer DUP is associated with a poorer prognosis (Cechnicki, Hanuszkiewicz, Polczyk, et al., Reference Cechnicki, Hanuszkiewicz and Polczyk2011), and therefore, it is critical that this group is provided with adequate care when they eventually do present. In certain cases, this may mean a hospital admission is the most appropriate course of action, but if so, they should be admitted with a clear rationale and for as brief a period as is necessary. For patients who are not admitted, again, there must be a solid outpatient alternative in place. For those who present more insidiously, this can be a challenge, as they may not necessarily fit into any of the defined treatment programs available; that is, they may not present acutely enough to meet criteria for an acute day hospital but may also be deemed ineligible for a rehabilitation service for patients with chronic illness. Ongoing development of community services as alternatives to admission needs to ensure that this group is taken into account.
Model of care
For some individuals presenting with FEP, inpatient care is a requirement, particularly for those who are at risk of harm or significant deterioration. However, there is also a considerable proportion of individuals for whom inpatient care is not appropriate, and for these individuals, it is important that the community-based services available to them are adequately resourced. The duty of care in FEP involves several aspects, including physical investigation (Dorney & Murphy, Reference Dorney and Murphy2021), careful risk management (Nordentoft, Madsen, & Fedyszyn, Reference Nordentoft, Madsen and Fedyszyn2015), and close medication monitoring (Dixon & Stroup, Reference Dixon and Stroup2015). These treatment targets are often more easily accessible in an inpatient setting, and the Australian Survey of High Impact Psychosis, in fact, found that the proportion of patients with psychotic disorders receiving annual physical examinations and blood tests has fallen over the years, posited to reflect the transition away from inpatient care (Morgan, Waterreus, Carr, et al., Reference Morgan, Waterreus and Carr2017). This may be, in part, why clinicians continue to lean toward admissions in certain areas. Thus, there is a balance to be struck. If we continue to develop our understanding of factors that drive hospital admissions and identify factors that may be modifiable, we can reduce unnecessary admissions and subsequently invest more in specialized outpatient clinics and assertive outreach programs. Continued investment in community-based services should aim to facilitate the provision of high-quality care in the community, including, for example, access to physical screening and monitoring at this crucial early stage.
Future research
The overarching aim in this area is to continue to reduce institutionalization, the risk of which starts with the index admission. In FEP, there are several factors potentially influencing the treatment trajectory from the point of first presentation. To further increase our knowledge around this, it would be useful to obtain a more detailed and up-to-date understanding of different views on the advantages and disadvantages of inpatient versus outpatient treatment at the outset. Perspectives should be sought from the array of stakeholders often involved in the early admission process, including psychiatric clinical staff (hospital- and community-based), primary care physicians, police officers, and, essentially, the patients and families themselves. It would also be important to identify whether other service factors are influencing decisions regarding admission, for example, varying levels of capacity in both inpatient and outpatient services. Regarding patient demographics, there were insufficient data for this review to conduct a sub-analysis on ethnicity or migrant status. It would be useful to have a broader understanding of these factors in relation to early admissions, given what we do know about the significance of ethnicity in admissions throughout the course of a psychotic illness and different pathways to care (Mann, Fisher, & Johnson, Reference Mann, Fisher and Johnson2014). As research in this area continues, we must also recognize the circumstances under which admission is appropriate and how to optimize inpatient care in this population, if required, with a robust and timely transitional plan to community services thereafter. With the ongoing drive to enhance outpatient alternatives to admission, potential obstacles to effective community care and engagement should be examined and addressed to ensure the provision of a high standard of early treatment in FEP.
Conclusions
Results demonstrate that over half of the people are hospitalized when they first present for FEP, a high proportion, with consequences for individuals and health services at large. First service contact must be prioritized as an opportunity for appropriate intervention, to either avoid unwarranted hospitalizations, or if hospitalization is required, to ensure the application of focused therapeutic objectives within intended timeframes.
Supplementary material
The supplementary material for this articlecan be found at http://doi.org/10.1017/S0033291725101256.
Acknowledgments
Diarmuid Stokes, College Liaison Librarian at University College Dublin.
Authors from whom responses were received in relation to requests for further data or clarification:
Miriam Fornells Ambrojo (Fornells-Ambrojo, Pocock, Mintah, et al., Reference Fornells-Ambrojo, Pocock and Mintah2018), Chan Sherry (Wong, Chan, Lam, et al., Reference Wong, Chan and Lam2011), James Stone (Rammou, Fisher, Johnson, et al., Reference Rammou, Fisher and Johnson2019), Philipp Baumann (Baumann et al., Reference Baumann, Crespi and Marion-Veyron2013), Nicholas Breitborde (Breitborde, Bell, Dawley, et al., Reference Breitborde, Bell and Dawley2015), Ashley Weiss (Weiss, Steadman, Samberg, et al., Reference Weiss, Steadman and Samberg2022), Ann Shinn (Shinn, Bolton, Karmacharya, et al., Reference Shinn, Bolton and Karmacharya2017), Jennifer Humensky (Humensky, Nossel, Bello, et al., Reference Humensky, Nossel and Bello2021), Joseph Boden (Turner, Boden, & Mulder, Reference Turner, Boden and Mulder2013), Robert Bota (Bota, Sagduyu, Munro, et al., Reference Bota, Sagduyu and Munro2005), Lisa Dixon (Humensky et al., Reference Humensky, Nossel and Bello2021), Paolo Fusar Poli (Fusar-Poli, De Micheli, Chalambrides, et al., Reference Fusar-Poli, De Micheli and Chalambrides2019; Fusar-Poli, Díaz-Caneja, Patel, et al., Reference Fusar-Poli, Díaz-Caneja and Patel2016; Fusar-Poli, Micheli, Patel, et al., Reference Fusar-Poli, Micheli and Patel2020), Jouko Miettunen (Miettunen, Lauronen, Veijola, et al., Reference Miettunen, Lauronen and Veijola2006), Rosa Ayesa Arriola (Ayesa-Arriola et al., Reference Ayesa-Arriola, Rodríguez-Sánchez and Morelli2011), Wing Chung Chang (Chang et al., Reference Chang, Lau and Chiu2016), Maite Arribas (Arribas, Solmi, Thompson, et al., Reference Arribas, Solmi and Thompson2022), Sheri Oduola (Oduola et al., Reference Oduola, Craig and Morgan2021), Martino Belvederi Murri (Belvederi Murri et al., Reference Belvederi Murri, Bertelli and Carozza2021), Sarah Keane (Keane et al., Reference Keane, Szigeti and Fanning2019), Ross Norman (Norman, Malla, Manchanda, et al., Reference Norman, Malla and Manchanda2005), and Kelly Anderson (Kurdyak et al., Reference Kurdyak, Mallia and de Oliveira2021).
Author contribution
L.G. and B.O’D. were responsible for the conception and design of the review. L.G. had overall responsibility for the management of the review. L.G. and V.T. screened and finalized the selection of studies and extracted data independently from included studies. L.G. and B.O’D. were responsible for data analysis and interpretation. L.G. was responsible for drafting the initial version of the manuscript. S.O., S.M., F.M., and M.C. reviewed and recommended edits to the manuscript. L.G. revised the final version.
Funding statement
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Competing interests
The authors declare none.







